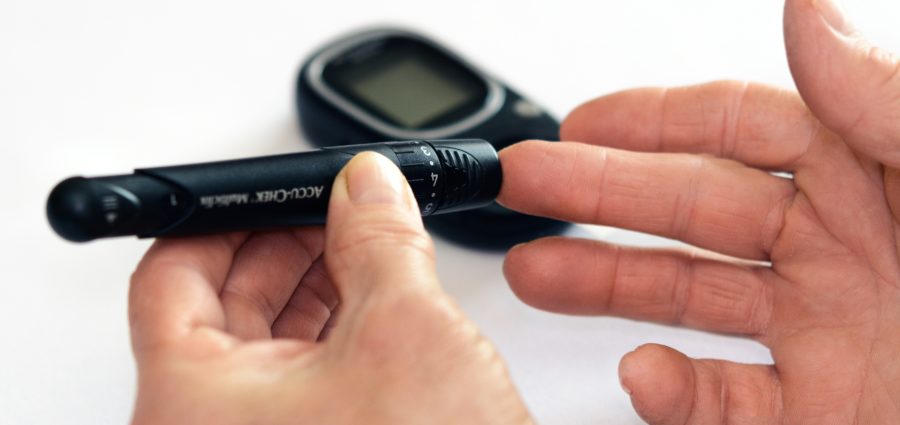
Type-2 diabetes now strikes adults in their prime – and Hispanics and Latinos may be among the most impacted by this trend.
According to the American Diabetes Association, here, almost one in 10 adult New Yorkers have diabetes, and diabetes has increased 13 percent in New York City since 2002. Almost 20 percent of Latino and Hispanic New Yorkers have diabetes. In New York City during 2007, 23 of every 100,000 Hispanics or Latinos died from diabetes. Contributing to this epidemic? Our soaring rates of obesity.
“Diabesity” is a preventable but deadly disease. Excess weight destroys the body’s ability to process sugar properly, with life-threatening consequences. While you cannot change having a family history of diabetes, you can do something to combat other risk factors, such as being overweight or sedentary (inactive). If you or a loved one has diabetes, your doctor will suggest lifestyle modifications and may prescribe medications to control blood sugar levels.
The good news is, fighting diabesity also helps you reduce the risk of long-term complications, such as heart disease, stroke, kidney or nerve damage and vision problems. To get your diabesity under control, you will need to consider a number of factors, including exercise, proper nutrition, monitoring your blood sugar, and taking medications effectively so you can reduce the risk of long-term consequences and feel better.
Maife Santillan, registered nurse for the Visiting Nurse Service of New York (VNSNY) in Bronx, has advice to help you with all of the steps involved in managing diabesity. VNSNY is the nation’s largest not-for-profit home- and community-based healthcare agency.
UNDERSTANDING DIABETES
If you have diabetes, your body does not produce enough insulin, or your body does not respond well to insulin-an important hormone. Insulin helps your body move glucose from the foods you eat into your cells for fuel (energy). There are a variety of symptoms of uncontrolled diabetes, from fatigue to increased thirst and urination to slow wound healing. Blood sugar monitoring, healthy eating, exercise and taking doctor-prescribed medications properly are important steps in managing this chronic condition. “The VNSNY nurse care manager can help you to understand your treatment plan so you can follow it with confidence and improve your health,” says Santillan.
THREE STEPS TO BEAT DIABESITY
“If you’re overweight, eating poorly or exercising infrequently, don’t wait until you’re diagnosed with diabetes to make lifestyle changes,” advises Santillan. “There are three things you can manage now, whether you’ve got diabetes or not.”
1. Nutrition
This is the number one issue for someone confronting diabesity. “When a VNSNY nurse creates a care plan for the member,” explains Santillan, “he or she is going to focus first on diet.” When shopping and planning meals for someone with diabetes:
A caregiver should also make sure that a diabetic loved one has sugary items on hand in case of an emergency. “Always examine the refrigerator,” says Santillan, “and make sure that orange juice is present, and hard candy is kept at hand.”
2. Hydration
Water may be the secret weapon in weight loss, here, say researchers in the U.S. and Germany. Although the impact is modest and the findings are preliminary, the researchers say water consumption increases the rate at which people burn calories which could have important implications for weight-control programs. Drinking water packs a one-two punch for those with diabetes, since insulin dries out the natural moisture of the skin. “Make sure someone with diabetes drinks enough water,” advises Santillan. “Caregivers should check skin for dryness and encourage hydration.” He suggests filling a pitcher to the maximum daily requirement in the morning, dispensing water by the cupful, and making sure the pitcher is empty by bedtime. A minimum of 8 cups of total fluids is recommended in a day unless restricted by other medical conditions.
3. Exercise
Staying active is a critical part of keeping diabetes under control. Interval training – alternating between short periods of high-intensity exercise and longer periods of low-intensity training – can be done at all fitness levels. It burns more fat and calories than trekking along at a constant pace.
Research shows that exercising like this improves endurance, strengthens the heart and has positive effects on metabolism. If you go for a walk, power-walk for a minute or two every five minutes. A minimum of 30 minutes of exercise every day is recommended. If you jog, bike or swim, bump up the intensity every few minutes and sustain that pace for at least 60 seconds.
(Always check with your doctor before embarking on an exercise regime.)
To learn more about programs that can help you or someone you love cope with diabetes, visit VNSNY.org or call 800–675–0391.