The room is spacious, bright and cheery, with TV monitors mounted at each of the 40 individual stations. Some take care of their business while watching TV, a few read, most listen to their IPods. Interrupting the constant din are the starts and stops of the machines, measured in gurgles and moans.
At quick glance, one might think they’ve walked into an upscale health club in suburbia. Instead, it’s the St. Barnabas Hospital Dialysis Center in the Bronx, a renovated parking garage, where from 6 a.m. to 6 p.m. six days a week, 220 outpatients undergo hemodialysis three times a week, three to four hours at a time.
Dialysis keeps alive an estimated 354,000 Americans who suffer from end stage renal disease. Dialysis becomes an ongoing and integral part of their lives, with a kidney transplant the only hope for breaking the routine (and staying alive).
At the dialysis center, one of the few in the Bronx owned by a not-for-profit hospital (rather than a national chain), many of the patients present with co-morbidities like diabetes, obesity, hypertension and HIV. Patients range in age from their 20s to their 90s, with some being on dialysis for over 20 years – although the survival rate nationally after five years is 31.9 percent and just 9 percent after 10 years.
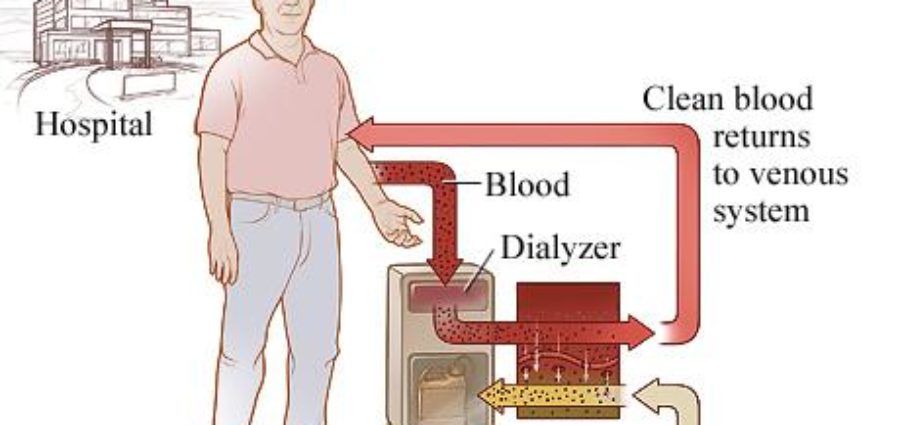
In hemodialysis, blood flows, a few ounces at a time, through a special filter that removes wastes and extra fluids. The machine then returns clean blood to the body with the harmful wastes, extra salt and fluids removed. This helps control the patient’s blood pressure and maintains the proper balance of chemicals like potassium and sodium in the body.
“Education is a big component of what we do here,” said Judy Rivere, a senior nurse. “We remind them constantly on what they can and cannot eat and teach them how to take care of themselves.”
It is not easy living on dialysis, but the staff at St. Barnabas makes it as positive an experience as possible. As a means to this end, they award prizes for answering monthly questions on such issues as kidney disease and diet, or for maintaining perfect attendance. Dialysis sessions become a social club of sorts for patients who maintain the same schedules week after week, month after month and even year after year. Friendships form, and patients often talk about stamping their medical ticket out of there (in the form of a kidney transplant). This was the case when a man in his 50s, a retired parks employee, recently returned triumphant to the center after receiving a transplant.
“It can be very motivating, but it won’t happen for everyone,” said Dr. James Croll, medical director of the facility. “After a transplant you need to take medicines so patients need to show they are compliant and otherwise healthy before a transplant can even be considered.”
About 15 or so patients here annually have transplants, either receiving kidneys from family members or cadavers with matching tissues.
Even beyond dialysis treatment, living with kidney disease is no walk in the park. Patients must maintain a very limited diet; this is especially difficult for the hospital’s many Latino patients, who tend to favor diets high in phosphorus (beans, plantains, chocolate, dairy products). In addition, they must keep their salt and potassium levels low (potassium is prominent in fruits like oranges, bananas and cantaloupes) and eat foods high in protein like egg whites, chicken, fish and turkey. Their fluid intake – including soup, fluid from fruit – cannot exceed 1 liter per day (or about ¼ glass).
Clinical dietitians at the St. Barnabas Hospital Dialysis Center work individually with patients, who often face restrictions further complicated by diabetes (which more than 40 percent have), obesity or hypertension.
Social workers like Joseph Kurian provide emotional support and counseling, and chase after patients who miss appointments. Failing to show for an appointment has serious repercussions: even one missed session can result in excess fluids in the lungs, bloating and even death.
“This is a difficult diagnosis. They may wake up one morning and decide they just can’t make it today,” said Kurian. “Many are depressed and we’re here to help them learn to cope with this, and we track them down when necessary. If they live alone, we see that someone is looking after them.”
Maritza Melendez knows about this. Having developed preeclampsia, a disease that affects both mother and child during pregnancy, she began to have health problems shortly after giving birth seven years ago to her second child. When she saw her doctor two years ago as a result of a substantial weight gain and chest pains, he immediately referred her to a nephrologist. She was told she needed to begin dialysis.
“I was scared to death. I thought I was going to die,” said Melendez, who was working at the time as an office manager at Monroe College. “At first I refused treatment, but after doing my own research I saw that this disease was treatable and not a kiss of death. People with this can live a long time.”
Dialysis was rough at first – her blood pressure dropped and one day, following treatment, she passed out after climbing three floors to her apartment. Generally healthy otherwise, Melendez soon fell into the routine of dialysis treatment and changing her diet. A year ago, she thought she had struck pay dirt when she was told a new kidney was waiting for her. However, when she learned the donator had hepatitis, she decided to wait for a better situation.
Today, Melendez is a member of the center’s patient advisory committee. In this capacity, she visits other patients when they are hospitalized and urges them to be compliant.
“Sometimes it carries more weight when you hear it from another patient,” she said. “Dialysis can be very tough, but a place like this brings up your spirits and motivates you. People here are generally upbeat. It may seem strange, but I actually look forward to coming here.”
On July 5, things took an even brighter turn for Melendez when she got the call she had long been waiting for – there was a match for a healthy kidney. She underwent surgery and today is doing well enough that she no longer needs dialysis.